Introduction
A lung transplantation is a surgical procedure where a damaged lung is replaced with a healthy one from a donor. It's usually reserved for patients with end-stage lung disease who have exhausted other treatments. Lung failure can be life-threatening due to inadequate oxygen delivery, but a successful transplant can significantly improve survival rates. Although the procedure has risks, it offers hope and improved quality of life for those with severe lung diseases.
Types of Lung Transplantation
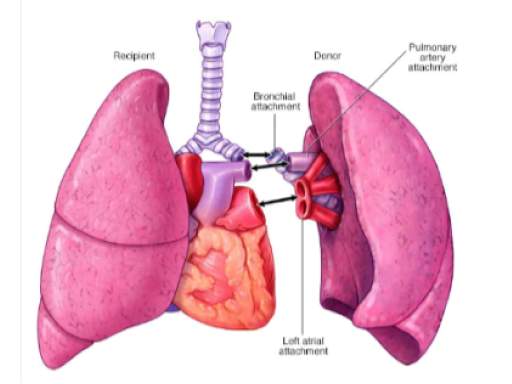
Single lung transplantation
This procedure involves transplanting a single lung.
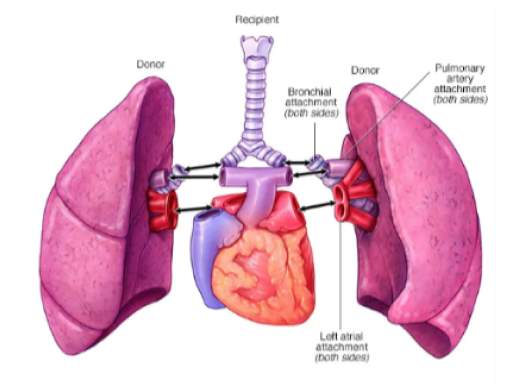
Double lung transplantation
This process involves transplanting both lungs. Both lungs are transplanted either in a single surgery or in sequential surgery. The procedure is known as a bilateral sequential transplant when it is sequential.
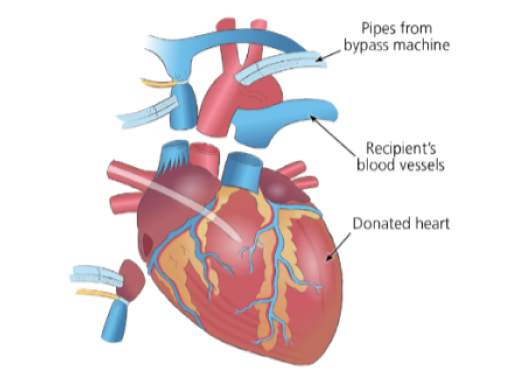
Heart & Double lung transplantation
This surgery involves the simultaneous transplant of the heart and lungs from a single donor.
We have some of the best specialty doctors from around the world, they bring years of experience and offer evidence-based treatment to ensure the best care for you.
Organ transplantation is considered a last resort and recommended only when the patient's organ condition becomes severe, life-threatening,and unresponsive to other medical treatments.
Our journey with you begins with an initial consultation where our pulmonologist will review your medical history, current symptoms, and perform a physical examination.
Our team will evaluate your heart, kidneys, liver, and other organs to ensure they can support the transplantation process and post-operative recovery.
Our team will provide comprehensive education about the transplantation procedure, potential risks, benefits, and the post-transplant care requirements.
After completing the evaluation process, our team will carefully review your case to determine if lung transplantation is the appropriate treatment option for you.
To assess your lung function and overall health, a series of diagnostic tests will be conducted, which may include pulmonary function tests, arterial blood gas analysis, chest imaging, and more.
Lung transplantation can be emotionally challenging, and we offer psychological evaluations to support you through the process.
If you are deemed eligible for lung transplantation, we will assist you in the process of placement on the transplant waiting list.
During the initial post-operative period, you will be closely monitored in our dedicated transplant unit. Our medical team will conduct regular assessments, including blood tests, X-rays, and lung function tests, to track your progress.
Our rehabilitation and physical therapy programs aim to help you regain strength, endurance, and function after surgery. We focus on enhancing your physical well-being and optimising lung function.
A balanced diet is crucial for post-transplant recovery. Our nutrition experts will work with you to develop a dietary plan that meets your nutritional needs and supports your healing process.
After discharge, regular follow-up appointments with our pulmonologists and transplant team are vital to ensure your ongoing health and monitor your lung function
To prevent rejection of the transplanted lung, you will need to take immunosuppressive medications. Our team will guide you on the proper administration and management of these medications to ensure their effectiveness and minimise side effects.
In the post-transplant period, you will be more susceptible to infections. We will provide comprehensive guidance on infection prevention measures to reduce the risk of complications.
Adjusting to life after lung transplantation can be emotionally challenging. Our dedicated team of social workers and psychologists will offer counselling and support to help you cope with these changes.
Living with a lung transplant
-
Follow-up: Visiting the hospital during the scheduled follow-up visit is important. The patient should not miss any follow-up visits. During the follow-up examination, the surgeon and respiratory specialist may look for signs of organ rejection, infection, or other complications.
-
Medications: Certain medications, such as antibiotics or analgesics, may be prescribed only for initial few days or weeks. However, some medications, such as immunosuppressants, may be required throughout life.
-
Healthy lifestyle: The patient should follow a healthy lifestyle that includes avoiding smoking, performing regular exercise, and undergoing routine immunisations.
As you recover from your transplantation, we'll closely monitor your health for any possible complications. Initially, you'll have weekly hospital visits, which will become less frequent over time. We may conduct tests like chest X-rays, pulmonary function tests, bronchoscopy, and chest CT scans at specific intervals.
Recovery time after lung transplantation varies, usually spanning several months to a year. Successful recovery relies on close monitoring and following post-transplant care guidelines diligently.
The waiting period for a lung transplant can vary widely based on the patient's blood type, the severity of their condition, and the availability of suitable donor organs. Typically, the waiting period can range from a few weeks to several months.
There is no strict age limit for lung transplantation. Both adults and children can undergo the lung transplant procedure, depending on their medical condition and suitability. Eligibility is determined on a case-by-case basis by a medical team. However, a recipient of age 65 years or less is seen to have better results.
Lung transplant recipients should be aware of risks such as organ rejection, infections, medication side effects, and post-surgical complications. Understanding these risks is crucial for making informed decisions and achieving optimal outcomes.
For a foreign national to undergo a lung transplant in India, the following rules apply: They must be registered with a transplant hospital in India and share their information with NOTTO. The Authorisation Committee assesses their eligibility and considers factors like medical urgency, visa validity, affordability, and ties to India before making a decision.
The cost varies depending on multiple factors. For an accurate quote, meeting with the transplant coordinator is best.
A lung transplantation is a surgical procedure in which a diseased or damaged lung is replaced with a healthy lung from a donor. There are two main types of lung transplants: single lung transplant, where one lung is replaced, and double lung transplant, where both lungs are replaced. The transplantation aims to improve lung function and quality of life for the recipient, but it involves careful evaluation, matching with a suitable donor, and post-transplantation care to ensure the best possible outcomes.
The lifespan of a transplanted lung varies among individuals. On average, most recipients can expect their transplanted lungs to function well for about 5 to 10 years. Nevertheless, advancements in surgical techniques, post-transplant care, and immunosuppressive medications have led to cases where transplanted lungs have functioned for over 15 years.
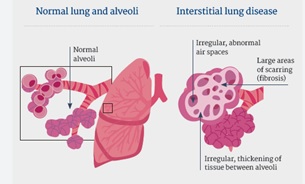
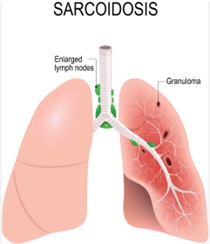
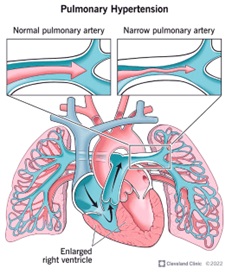
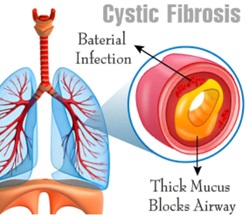
Individuals eligible for lung transplantation have severe, irreversible lung diseases like idiopathic pulmonary fibrosis (IPF), cystic fibrosis (CF), pulmonary hypertension, or chronic obstructive pulmonary disease (COPD). The decision is based on factors such as disease severity, overall health status, and the absence of contraindications.
Certainly! After undergoing lung transplantation, it is crucial to implement lifestyle changes to ensure the long-term success of the transplant. These modifications may involve strict adherence to a medication regimen, adopting a healthy diet, regular exercise, avoiding tobacco smoke and environmental pollutants, and practising good hygiene to minimise the risk of infections. Following the guidelines provided by the transplant team is essential for recipients to achieve a healthy and prosperous outcome.
Let's hear from our patients