Death is one of the few certainties of life yet in India, it remains one of the least discussed amongst family and most importantly with the patient. For patients facing irreversible illness, silence can become a form of suffering.
When someone we love is seriously ill, conversations do happen but often around the patient, not with them. Families ask doctors:
● How much time?”
● Will this get better?”
● Can nothing more be done?”
But one phrase is carefully avoided: “end of life.” It feels too final. Too painful. Almost like giving up. And in that silence, an important voice is lost the voice of the patient.
Why Don’t We Talk to Patients About Death?
Families don’t stay silent out of neglect. They stay silent out of love.
● They may feel the patient shouldn’t know the full diagnosis
● They worry that truth will destroy hope
● They fear that talking about death might somehow “bring it closer”
● They simply don’t know how to begin such a conversation
● And above all, they want to keep fighting for as long as possible
But in trying to protect the patient, we sometimes leave them out of decisions about their own life. Treatments, ICU admissions, and life support choices are often decided without asking:
“What would you want?”
What Medicine Tells Us
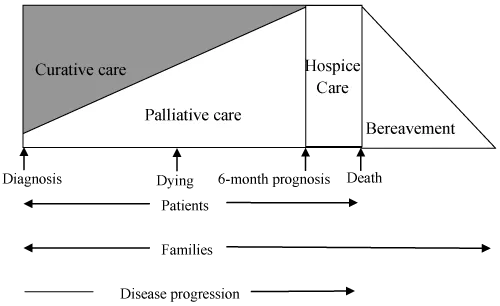
Palliative care offers a different way of looking at this. Palliative care is not about giving up. It is about focusing on quality of life when cure is no longer possible. It prioritizes relief from pain and suffering, honest communication, and care that aligns with the patient’s values and wishes, while being inclusive of the care givers emotions and connections with the patient that in all circumstances influence the decisions taken, especially at the end of life.
At its heart is one simple truth: The patient should be at the center of decisions.
What Does “End of Life” Really Mean?
There is a common misunderstanding that “end of life” means the last few hours. It doesn’t.
● End of life begins when an illness is no longer curable, and the focus shifts to comfort and dignity. This phase can last weeks or even months.
● The final hours of the End of Life are called active dying.
This means conversations shouldn’t happen at this very last moment they should begin earlier, while the patient can still express their wishes. While as a family we can bring to focus what matters to the patient, completing 'unfinished business', family togetherness, memories and legacies spoken and made.
What the Law in India tells us:
India’s legal system now clearly supports the fact that patients have a say in how they wish to be treated at the end of life.
Over the years, the Supreme Court has made important decisions:
● It recognized that the right to life includes the right to die with dignity (Article 21)
● It allowed people to write living wills (advance directives) documents that state their wishes about medical care, when they are no longer able to voice their wishes.
● It legalized passive euthanasia, better understood as:
Withholding of life sustaining treatment: A decision made not to initiate or escalate a life-sustaining treatment in terminal illness in accordance with expressed wishes of the patient or surrogate.
Withdrawal of life sustaining treatment: A decision made to cease or remove a life sustaining intervention in terminal illness in accordance with expressed wishes of the patient or surrogate
These are focused on "ALLOWING A NATURAL DEATH", when recovery is no longer possible, NOT as ending a life as commonly misunderstood.
The message is clear: The patient’s voice matters.
Are Medicine and Law aligned?
Yes, they are aligned.
Both emphasize:
● Dignity as a priority for the patient
● Relief from suffering as paramount- providing quality in death and dying.
● Respect for patient choices - validating that the patient voice that is not always heard - NOW needs to be.
But in real life, however, challenges remain:
● Families struggle to have these important conversations
● Many individuals are unaware of living wills
● Cultural values often prioritize family decisions over individual patient choice
Bringing the Patient Back into the Conversation
Here is what Palliative Care wishes and advocates for the patient and their families:
Talking about death is never easy. It feels uncomfortable, emotional, and sometimes even frightening. But these conversations are essential and are not about taking away hope.
Palliative care team at ASTER HOSPITALS help families and patients have these conversations with honesty and compassion.
The right to die without suffering is not about choosing death over life.
It is about choosing:
● Dignity over unnecessary suffering from life prolonging measures.
● Comfort over invasive treatments
● Patient being heard at all times.
The law has created a framework. Medicine supports it.
Because the real question is not: “Shall we talk about death?” It is: “Can we afford not to talk about it?”
Conversations at the End of Life - are about changing what hope looks like.
● About comfort of the patient
● About asking the patient how they wish to be treated at the end of life and where they wish to be treated.
● About a Living Will/ Advanced Medical Directive
● About being at home - understanding the support that can be continued when care extended home - at ASTER it is through ASTER CARE EXTENDED.
● About having symptoms controlled to the best extent possible through support from the Palliative specialists at ASTER PAIN AND PALLIATIVE TEAM.
● About being surrounded by loved ones - Educating the family on how to support patient at home, without a feeling of abandonment.
If you are reading this - and you are a patient of the loved one of a patient who is is suffering from a life limiting illness, now been offered comfort care, please come and meet us as ASTER CMI HOSPITAL - PAIN AND PALLIATIVE DEPARTMENT and we would be there to have an open conversation with you.