Mrs. K, a 60 year old lady presented to the hospital with complaints of whole body pain, constant moaning, minimal food intake, constant tremors, inability to communicate with family, bedbound. Symptoms had been worsening for 3 years, but rapidly progressing over the past 3 months. She was diagnosed of a life limiting illness 1 year ago.
Mrs. K had been a fiercely independent lady, who had been the backbone of her family.
The family – they were unsure if they were caring for her the right way. Unsure of the future and the fear that she would be in constant agony and suffer at the end of her life. What should they do?
These are queries which are increasingly familiar to many. How do I care for my loved one? Where should I provide the care? What should I be aware of?
Before we go ahead, there are a few terms that need to be understood:
Life limiting illness – A term used to describe an incurable condition that will shorten a person’s life, though they may continue to live active lives for many years
Terminal illness – An irreversible or incurable disease condition from which death is expected in the foreseeable future.
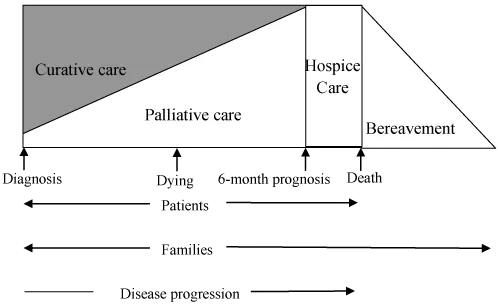
End of life care – An approach to a terminally ill patient that shifts the focus of care to symptom control, comfort, dignity, quality of life and quality of dying rather than treatments aimed at cure or prolongation of life.
Symptoms - The difficulties faced by the patient during the treatment that affect the quality and dignity of life
Let us first understand what Palliative Medicine/Care is -
Palliative Medicine is Specialty field in Medicine, that addresses the needs of the patient and family. The patient being anyone who is suffering from a life limiting illness, affecting the quality and dignity of their life.
You may ask - How is it different from the other fields of Medicine?
Palliative medicine works on the “Holistic Care” principle, that a person suffering has experiences in different facets of their being. The physical, emotional, psychological, spiritual, financial facets that affect the individual in entirety. This is called “Total Pain”. The family of the patient goes through a similar experience. Hence, Palliative medicine cares for both the patient and the family.
Palliative Care is provided in the hospital, at home and in a Hospice by a Palliative Medicine Specialist.
The care is provided by a team of professionals who work together as a single team to provide a personalized care. Continued care at home is provided through ASTER EXTENDED CARE SERVICES.
Hospice care is used synonymously with Palliative care and equated at all levels with it. This is not true. Let us go through the differences, that will help you understand it more:
Who is eligible for this care?
Palliative Medicine
- Any patient who is diagnosed with a life limiting illness.
- Care begins at the time of diagnosis.
- Care offered alongside the curative treatment by the primary treating doctors.
- Symptoms management after assessment.
- The care for not limited to any particular phase in a patient’s illness.
- The family provide the bigger portion of the care
Hospice care
- Hospice care is provided during the terminal stages of the life (last months) of a patient with a life limiting illness.
- The Palliative Team provide symptom control as patient progressively declines, giving them symptom and supportive care at the terminal stage.
- The care is provided to both the patient and family.
- The professional team provide a bigger portion of the care
What illness is called life limiting?
- Any illness that decreases the life span of a person prematurely is called a life limiting illness.
- Chronic kidney disease leading to End stage renal failure, Cardiac failure.
- Lung diseases such as COPD/ Interstitial lung disease, Cancer.
- Neurological conditions such as Parkinson’s disease/ Dementia/Stroke/ Motor Neuron Disease.
Is it age limited?
- Specialist Palliative care is provided to all ages, from neonates, children, adults and elderly
What is the care provided?
Palliative Medicine
- Specialist Palliative Physicians are trained in identification, assessment, diagnosis and evidence- based management of symptoms, from the time of diagnosis and continued throughout the disease trajectory.
- Communication of the treatment options.
- Provide best Interdisciplinary care to improve the quality of life and dignity of life of patient and family.
- Communication and accurate guidance at decision making, through the disease trajectory, especially at the end of life.
- Integration of the holistic care of the patient and extend the care to be provided in a home setting.
- Care of the patient at end of life. # Provide Quality and dignity of death.
- Care for the bereaved family.
Hospice care
- Specialist Palliative Care enabling good holistic support and care, of the distressing symptoms of a patient nearing the end of life. # The Hospice also provides respite care. (To avail pure hospice care the acceptance of the family is essential that the decline in clinical condition will ultimately lead to the demise of the patient with minimal intervention medically)
Who makes up the team?
Palliative Medicine
- Specialist Palliative Physician,
- Nurse
- Psychologist
- psycho-oncologist
- Nutritionist
- Pharmacologist
- Physiotherapist
- Occupational Therapist
- Speech and language therapist
- Volunteers
- Play
- therapists
- spiritual leaders
Along with the primary treating teams.
Hospice care
- Specialist Palliative Physician
- Nurse
- Psychologist
- psycho-oncologist
- Nutritionist
- Physiotherapist
- Occupational Therapist
- Volunteers
- Play therapists
- spiritual leaders
Where is it provided?
Palliative Medicine
- Hospital (Outpatient & Inpatient)
- Home
- Through telephone conversations At Care Home facilities (in
- consultation with a Palliative Care specialist)
Hospice care
- Hospice
- Home
In summary, please remember that if your loved one is suffering from a life limiting illness, palliative medicine specialist in Bangalore is there to support your loved one and you from the time of diagnosis. We care for your loved one alongside your Primary Physician. The care in provided in the hospital setting, through ASTER EXTENDED CARE SERVICES at home and can also be provided at a Hospice.
Hospice however provides Specialist Palliative Support during the terminal phase of life, providing quality of death.