Finest hands working in unison, to get you back on your feet.
The Orthopaedics Centre covers the full spectrum of bone, joint, and spine disorders. Our hospitals are well-equipped to tend to all sub-specialities of orthopaedics under a single roof, helping you get back on your feet in the minimum possible time.
Our exceptional team of doctors have vast experience in all orthopaedic subspecialties including trauma and orthopaedic surgery, joint replacement, wrist, upper limb & shoulder care, paediatric orthopaedics and deformity correction, orthopaedic oncology, spine, sports medicine, rheumatology and microvascular surgery. Multidisciplinary in approach, they provide holistic, evidence-based treatment to patients, with the support of speciality-trained nurses, physical medicine, and rehabilitation physicians.
Our impeccable record and success stories stem from the cutting-edge techniques we follow, our steadfast adherence to world-class standards, and our pre-eminent team of experts who are highly versed in clinical and surgical abilities.
Our doctors go well beyond and deliver a 360-degree swathe of services under one roof.
We take pride in stating that our results are amongst the very best in the country.
Our Specialities
Through our 25+ specialities, we provide in-depth expertise in the spectrum of advance medical and surgical interventions. Our specialties are integrated to provide a seamless experience.
Advanced Technology & Facilities
Well equipped with the latest medical equipment, modern technology & infrastructure, Aster Hospital is one of the best hospitals in India.
Arthrography
Bone scans
Discography
CT and MRI
Electromyography
X-ray
Blood tests
Bone scan
Operation Theatre equipped with Laminar Air flow.
Post operative pain control by epidural and IV analgesia by a team of experienced anaesthesiologists
State of the art Instrumentataion.
Image Intensifiers
Well equipped ICU for post operative care.
Lead ECG
2D and 3D Echocardiography including colour Doppler and contrast ECHO
Strain Imaging - Speckle Tracking and Heart Model
Trans-oesophageal Echocardiogram (TEE) / Dobutamine Stress Echo
Treadmill test (TMT)
Holter - 24 hrs and 48 hrs
Event monitoring and loop recorders
Ambulatory blood pressure monitoring (ABPM)
Head-up tilt table test (HUTT)
Pacemaker check and programming
Cardiac CT including CT coronary angiogram
Latest monoplane & bi-plane cathlab
Cardiac MRI including stress adenosine protocol
Aster Medcity offers world-class inpatient care to its patients, with the support of an award-winning team of Nurses, Therapists and Technicians.
Wards, double rooms, standard rooms, executive rooms, deluxe rooms presidential suites
Dedicated Cardiac ICU
Independent ICUs with a view that minimise chances of infection and ICU psychosis
Dedicated cardiac surgery suites
Advanced infection control facilities
State-of-the-art cardiac imaging
• Whole body bone scan
• Regional three-phase bone scan
• Regional infection imaging
• Bone graft viability
• Lymphoscintigraphy
• Regional infection PET imaging to diagnose osteomyelitis in patients
who have undergone hip replacement surgeries
• Strontium therapy for bone pain palliation
• Needle Biopsy
• Soft tissue and bone pathology
• Immunohistochemistry
• Frozen section
• Orthopaedic rehabilitation for musculoskeletal injuries and disorders
• Rehabilitation for patients who have undergone surgeries, including amputees
• Rheumatological rehabilitation with focus on prevention of functional disorders, improving movement and management of pain / stiffness
• Sports rehabilitation
• Orthotic & prosthetic management
• Hand rehabilitation post fracture, injury or surgery
ORI Fusion Digital Integrated Operation Theatres With 22 Operating Rooms that are on par with some of the largest in the world, Aster Medcity, for the first time South India, introduces ORI Fusion Digital Integrated Operation Theatres using Karlstorz OR1 Fusion - Asia Pacific’s first complete digital integration system.
The integration enables real-time sharing of images, videos and medical reports, which not only facilitates virtual participation from any location in the world, but also helps the rest of the surgical team to monitor the patient closely during the operative procedure, much to the benefit and safety of the patient undergoing the surgery.
Aster Medcity is also the first surgical facility in the state to offer Robotic Surgery using high-precision da Vinci Surgery Robot.
We combine our expertise in the areas of patient-care, clinical research and academics in order to provide the highest level of specialised services to our patients. The Aster spine center was conceived as part of the overall scope of neurosurgery and was incorporated into our original vision document. As part of the transformation into a global COE a dedicated aster spine center was proposed. This would be a multispeciality service including neurosurgical and orthopaedic spine surgeons covering the entire gamut of spine pathology, both elective and emergency. The primary spine service would be supported by a very active physical medicine and rehabilitation service, and other departments like neurology, endocrinology, radiology and oncology. It might be possible to include an element of holistic care into the spine center by association with indigenous systems of medicine like Ayurveda.
- OR1 Fusion Digital Integrated Green OT certified surgical Suites
- IntelliSpace Critical Care and Anaesthesia (ICCA) ICUs
- Level 3 PICU
- 3.0 Tesla Widebore MRI
- 256 Slice Philips iCT Scan
- DEXA for bone density measurement
- Philips Astonish True Flight Select
- PET-CT with Time Of Flight Technology
- GE SPECT-CT Optima NM 640 Gamma Camera>
- True Beam Linear Accelerator with FFF Technology
- Karl Storz Endoscope
- Siemens Isocentric 3D C-arm
- Medtronic Stealth Station Navigation System
- Leica M530 OH6 Operating Microscope
- Leica M525 OH4 Operating Microscope
- Medtronic Legend high-speed pneumatic drills
- Medtronic Legend EHS Stylus electric drills
- Medtronic Legend oscillating and reciprocating microsaws
- Intraoperative Bone CUSA
- Intraoperative electrophysiological monitoring
- Allen Spine System Table
- Needle biopsy
- Soft tissue and bone pathology
- Spine and peripheral nerve pathology
- Immunohistochemistry & frozen section
- Advanced navigation system
- Endoscopy and MISS systems
- Intraop MRI
- Gamma (SPECT) Camera
- Whole body bone scan
- Regional three-phase bone scan
- Regional infection imaging
Robotic-assisted knee replacement surgery is an advanced surgical technique that utilizes robotic technology to assist surgeons in performing total or partial knee replacement procedures with enhanced precision and accuracy. This technology allows for a more personalized approach to knee surgery, potentially resulting in better outcomes and faster recovery times for patients.
FAQs
Want to find out more about the treatment? The answer to your questions can be found below.
When should a joint be replaced?
Moderate to severe arthritis interfering with daily activities.
What is a neglected fracture?
A neglected fracture is a type of bone break that has not received timely or appropriate medical treatment, resulting in delayed or insufficient healing. This delay often leads to complications and poses challenges in the management of the fracture, potentially affecting the overall outcome of treatment.
What are the potential complications of neglected fractures?
Complications associated with neglected fractures encompass a range of issues. These may include malunion, where the fractured bone heals in an improper alignment; non-union, indicating a failure of the bone to heal; deformities that affect the shape or structure of the bone; chronic pain; limited joint motion; and an increased risk of infection due to the prolonged exposure of the fracture site.
What treatment options are available for neglected fractures?
The treatment of neglected fractures is individualized based on the specific characteristics of the fracture. Surgical intervention may be required, involving procedures such as fracture reduction, fixation using implants, or bone grafting. Physical therapy and rehabilitation play a crucial role in restoring functionality, and the treatment plan may be more complex than for fractures addressed promptly.
What challenges may arise in the treatment of neglected fractures?
Addressing neglected fractures poses unique challenges. These challenges may include correcting bone deformities resulting from delayed treatment, managing complications such as infections that may have developed over time, and achieving stable fixation during surgical procedures. Additionally, the rehabilitation process may be more prolonged, and patients may require additional support and monitoring.
What conditions can be treated with shoulder arthroscopy?
Shoulder arthroscopy is versatile and can address conditions such as rotator cuff tears, labral tears, shoulder impingement, frozen shoulder, and recurrent dislocations. Its dual diagnostic and therapeutic capabilities make it a valuable tool for orthopedic surgeons.
What are the benefits of shoulder arthroscopy over traditional open surgery?
Shoulder arthroscopy offers several advantages, including smaller incisions, reduced damage to surrounding tissues, faster recovery times, and decreased postoperative pain. Patients often experience improved range of motion and function with this less invasive approach.
Are there risks associated with shoulder arthroscopy?
While shoulder arthroscopy is considered safe, potential risks include infection, bleeding, nerve injury, or stiffness. However, the overall complication rate is relatively low, and the benefits of the procedure often outweigh the risks.
What knee conditions can be addressed with arthroscopy?
Knee arthroscopy is suitable for treating a range of conditions, including meniscal tears, ligament injuries like ACL tears, cartilage damage, and synovitis. The procedure allows for both diagnostic assessment and therapeutic interventions.
What are the advantages of knee arthroscopy?
Knee arthroscopy offers several advantages, including smaller incisions, reduced scarring, faster recovery times, and less postoperative pain compared to open knee surgery. The minimally invasive approach allows for targeted treatment of specific issues within the knee joint.
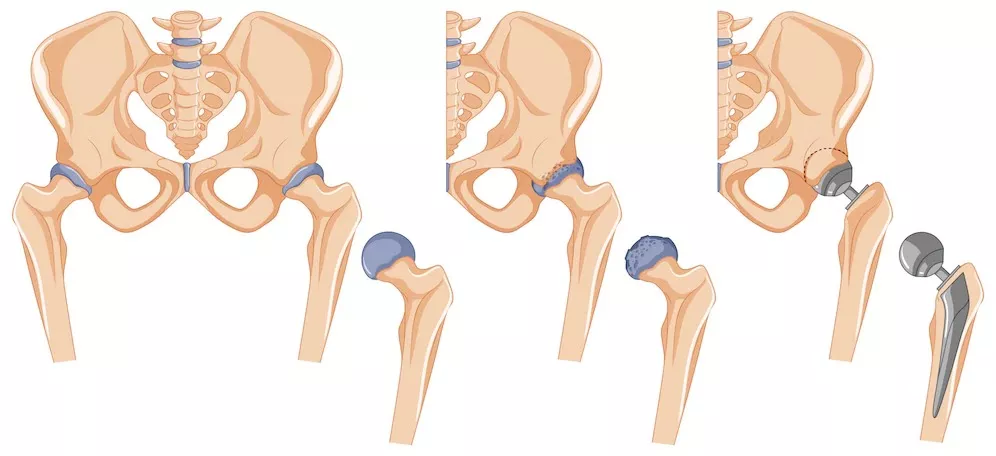
What is hip replacement surgery?
Hip replacement surgery, also known as hip arthroplasty, is a surgical procedure in which a damaged or diseased hip joint is replaced with an artificial joint, called a prosthesis, to relieve pain and improve mobility.
What are the types of hip replacement surgery?
There are several types of hip replacement surgery, including total hip replacement (replacing both the ball and socket of the hip joint), partial hip replacement (replacing only the ball portion of the hip joint), and hip resurfacing (reshaping the damaged bone and capping it with a metal prosthesis)
What are the potential risks and complications of hip replacement surgery?
Potential risks and complications of hip replacement surgery include infection, blood clots, dislocation, implant loosening or failure, nerve or blood vessel injury, and complications related to anesthesia. Patients should discuss these risks with their surgeon before undergoing surgery.
What activities can I do after hip replacement surgery?
Following hip replacement surgery, most patients can engage in low-impact activities such as walking, swimming, cycling, and golfing. However, high-impact activities or sports that involve running, jumping, or heavy lifting may need to be avoided to prevent implant wear or damage.
When can I return to work after hip replacement surgery?
The timing of returning to work depends on factors such as the type of work performed, the physical demands of the job, and the individual's rate of recovery. Most patients can return to light-duty or sedentary work within a few weeks to months after surgery, while those with physically demanding jobs may require a longer recovery period.
What are the risks of ceramic hip replacement?
Like other surgeries, ceramic hip surgery has some risks including:
- Reaction to anesthesia
- Infections
- Excessive bleeding
- Blood clots.
What are the symptoms of a multiligamentous knee injury?
Symptoms may include
- severe pain
- swelling
- instability or a feeling of the knee "giving way,"
- inability to bear weight on the affected leg, and limited range of motion.
What are the treatment options for a multiligamentous knee injury?
Treatment depends on the severity of the injury and which ligaments are involved. It may include conservative measures such as rest, ice, physical therapy, and bracing, or surgical intervention to repair or reconstruct the damaged ligaments.
Can I return to sports or physical activities after a multiligamentous knee injury?
With proper treatment and rehabilitation, many patients can return to their previous level of activity. However, it's crucial to follow the guidance of your healthcare provider and sports medicine team to ensure a safe return to sports or physical activities.
What is a growth factor injection for OA knee?
A growth factor injection involves the use of concentrated growth factors, typically derived from the patient's own blood (autologous), to promote healing and tissue regeneration in the knee affected by osteoarthritis.
What types of growth factors are commonly used in these injections?
Commonly used growth factors include
platelet-derived growth factor (PDGF)
transforming growth factor-beta (TGF-β)
insulin-like growth factor (IGF), and vascular endothelial growth factor (VEGF).
How is a growth factor injection administered?
The procedure involves
- Drawing a small amount of blood from the patient
- Processing it to concentrate the growth factors
- Then injecting the concentrated solution directly into the affected knee joint under sterile conditions, often guided by imaging techniques such as ultrasound.
How soon can patients expect to experience improvement after a growth factor injection?
The timeframe for experiencing improvement varies among individuals. Some patients may notice relief within a few days to weeks after the injection, while others may require more time to see significant benefits.
The duration of pain relief and improvement in symptoms can vary. Some patients may experience longlasting benefits for several months to years, while others may require periodic injections to maintain results.
What are some common conditions treated in the Orthopedic Department?
The Orthopedic Department treats a wide range of conditions, including musculoskeletal disorders, sports injuries, arthritis, and osteoporosis. They also provide care for pediatric trauma and manage acute orthopedic emergencies.
What are some of the major services offered by the Orthopedic Department?
The Orthopedic Department offers services like evaluation, diagnosis, and treatment of orthopedic conditions, surgical procedures, rehabilitation, and follow-up care. They also specialize in joint preservation procedures, hip and knee joint replacement/reconstruction, and minimally invasive fracture surgery.
How does the Orthopedic Department treat arthritis?
The Orthopedic Department provides both conservative and surgical management of arthritis. This includes lifestyle changes, medication, physical therapy, and in severe cases, joint replacement surgery.
How does the Orthopedic Department handle pediatric trauma?
The Orthopedic Department has a dedicated team of specialists trained in pediatric trauma care. They provide prompt and effective medical care to ensure the best possible outcome for children who have experienced a traumatic injury.
What is the role of the Orthopedic Department in geriatric orthopedics?
The Orthopedic Department provides personalized, age-appropriate care to older adults to help them maintain their mobility and independence. They understand that older adults have unique medical and physical needs, and they tailor their treatment plans accordingly.
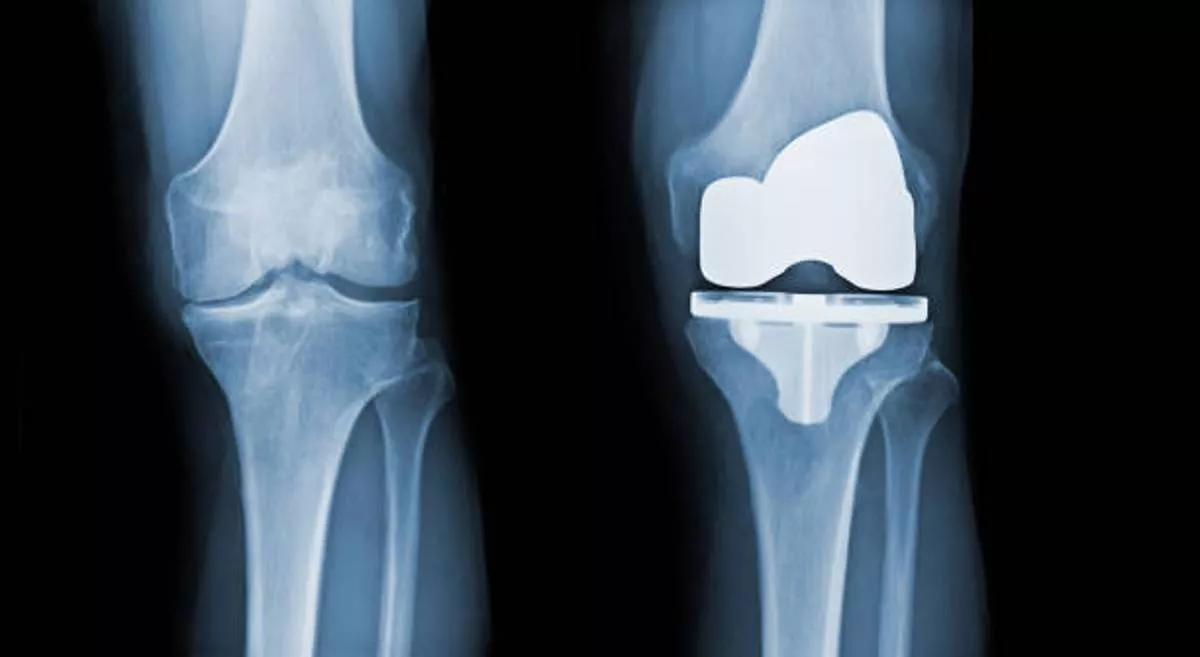
How is joint Replacement done?
In Arthritis, the damaged cartilage and bone from the joint are replaced with a prosthesis made of metal, polyethylene, ceramic, etc to regain normal joint biomechanics.
What are the common causes of neglected fractures?
Neglected fractures can arise from various factors, including delayed medical attention due to lack of awareness, financial constraints preventing immediate treatment, or limited access to healthcare facilities. Patients may neglect seeking timely treatment for fractures for reasons such as underestimating the severity of the injury or lacking knowledge about available healthcare options.
How do you diagnose neglected fractures?
The diagnosis of neglected fractures involves a comprehensive approach. It includes a detailed patient history, thorough clinical examination, and imaging studies such as X-rays, CT scans, or MRI. The suspicion of a neglected fracture arises when there is evidence of delayed medical attention or signs of improper healing in the imaging studies.
Can neglected fractures be treated successfully, even after a delay?
Neglected fractures can be treated successfully, even with a delay in seeking medical attention. However, the success of the treatment depends on factors such as the type of fracture, the extent of the delay, and the overall health of the patient. While early intervention generally yields better results, late treatment can still provide significant benefits in many cases.
What is shoulder arthroscopy?
Shoulder arthroscopy is a minimally invasive surgical procedure that utilizes a specialized camera called an arthroscope and small instruments to diagnose and treat various shoulder conditions. It provides a detailed view inside the shoulder joint without the need for large incisions.
How is shoulder arthroscopy performed?
During shoulder arthroscopy, small incisions are made, and the arthroscope is inserted to visualize the shoulder joint. Specialized instruments are then used to repair or treat issues identified during the procedure. This minimally invasive approach reduces trauma to surrounding tissues.
What is the recovery time for shoulder arthroscopy?
Recovery time varies based on the specific procedure and individual patient factors. Generally, patients can expect a quicker recovery compared to open surgery. Early initiation of motion exercises and adherence to a rehabilitation plan are crucial for optimal recovery.
What is knee arthroscopy?
Knee arthroscopy is a minimally invasive surgical technique that employs a small camera and specialized instruments to diagnose and treat various knee conditions. It is commonly utilized for issues such as meniscal tears, ligament injuries, and cartilage damage.
How is knee arthroscopy performed?
Knee arthroscopy involves making small incisions through which an arthroscope is inserted to visualize the internal structures of the knee. Specialized instruments are then used to repair or remove damaged tissues, enabling a faster recovery compared to traditional open surgery.
What is the typical recovery period for knee arthroscopy?
Recovery duration varies based on the complexity of the procedure and individual factors. Generally, patients can resume normal activities within a few weeks, with physical therapy playing a crucial role in restoring knee function and strength.
Who is a candidate for hip replacement surgery?
Candidates for hip replacement surgery typically have severe hip pain, stiffness, and mobility limitations due to conditions such as osteoarthritis, rheumatoid arthritis, hip fractures, or avascular necrosis that have not responded to conservative treatments.
What is the recovery process like after hip replacement surgery?
The recovery process varies for each individual but typically involves a hospital stay of 1-3 days followed by physical therapy and rehabilitation to regain strength, mobility, and function in the hip joint. Most patients can resume normal activities within a few weeks to months after surgery.
How long does a hip replacement last?
The lifespan of a hip replacement implant varies depending on factors such as the patient's age, activity level, implant materials, and surgical technique. Generally, most hip replacements last 15-20 years or more before requiring revision surgery.
Will I need physical therapy after hip replacement surgery?
Yes, physical therapy is an essential part of the recovery process after hip replacement surgery. Physical therapists will work with patients to improve strength, flexibility, and range of motion in the hip joint, as well as teach proper techniques for walking and performing daily activities.
How can I prepare for hip replacement surgery?
Patients can prepare for hip replacement surgery by following their surgeon's preoperative instructions, which may include lifestyle modifications, medication adjustments, preoperative testing, and planning for postoperative care and rehabilitation. It's essential to communicate openly with the surgical team and address any concerns or questions before the procedure.
What is a multiligamentous knee injury?
A multiligamentous knee injury involves damage to two or more of the major ligaments in the knee, such as the anterior cruciate ligament (ACL), posterior cruciate ligament (PCL), medial collateral ligament (MCL), and lateral collateral ligament (LCL).
These injuries often result from high-impact trauma, such as sports injuries, car accidents, or falls. They can involve direct blows to the knee or extreme twisting motions.
How is a multiligamentous knee injury diagnosed?
A comprehensive physical examination, along with imaging tests such as X-rays, MRI scans, or ultrasound, helps diagnose the extent of the injury and which ligaments are affected.
What is the recovery process like?
Recovery from a multiligamentous knee injury can be lengthy and requires patience and dedication to rehabilitation exercises. The timeline varies depending on the severity of the injury and the chosen treatment approach.
How can I prevent a multiligamentous knee injury?
Preventive measures include maintaining strength and flexibility in the muscles around the knee, using proper techniques during sports or physical activities, wearing appropriate protective gear, and avoiding risky movements or situations that could lead to injury.
How does a growth factor injection work?
The growth factors contained in the injection stimulate the body's natural healing processes, encouraging the repair of damaged cartilage, reducing inflammation, and potentially slowing down the progression of osteoarthritis.
Who is a suitable candidate for growth factor injection in the OA knee?
Patients with mild to moderate osteoarthritis of the knee who have not responded adequately to conservative treatments such as physical therapy, medication, and corticosteroid injections may be candidates for growth factor injections.
What are the potential benefits of growth factor injection for OA knee?
Benefits may include reduced pain, improved function and mobility, decreased inflammation, and potential regeneration of damaged cartilage, leading to long-term relief and improved quality of life.
What is the Orthopedic Department at Aster Whitefield Hospital?
The Orthopedic Department at Aster Whitefield Hospital provides high-quality care and treatment to patients with musculoskeletal disorders. This includes conditions that affect the bones, joints, ligaments, tendons, and muscles.
What diagnostic tests are conducted by the Orthopedic Department?
The Orthopedic Department conducts various diagnostic tests such as X-rays, MRI, CT scans, or ultrasound to accurately diagnose the underlying condition.
What types of surgical procedures are performed by the Orthopedic Department?
The Orthopedic Department performs a variety of surgical procedures, including arthroscopy, ligament reconstruction, joint replacement, and deformity correction.
What is the approach of the Orthopedic Department towards sports injuries?
The Orthopedic Department provides comprehensive care for sports injuries, including diagnosis, treatment, and rehabilitation. They also perform arthroscopy and ligament reconstruction for sports-related injuries.
What is the approach of the Orthopedic Department towards osteoporosis management?
The Orthopedic Department manages osteoporosis through a combination of lifestyle changes, medication, and in some cases, surgery. They aim to prevent the progression of bone loss and reduce the risk of fractures.
Patient Stories
Our patients are our best advocates, hear the inspiring stories of their treatment journey
Blogs
The source of trustworthy health and medical information. Through this section, we provide research-based health information, and all that is happening in Aster Hospital.
News & Events
Stay updated with the latest happenings at Aster Hospitals. Explore our News and Events section for insightful articles, health tips, upcoming events, and noteworthy achievements.