A complex case of Dissecting Aneurysm of Aorta was treated successfully by a multi-disciplinary team exemplifying the need for cooperation and interdependence of various departments in handling difficult clinical situations.
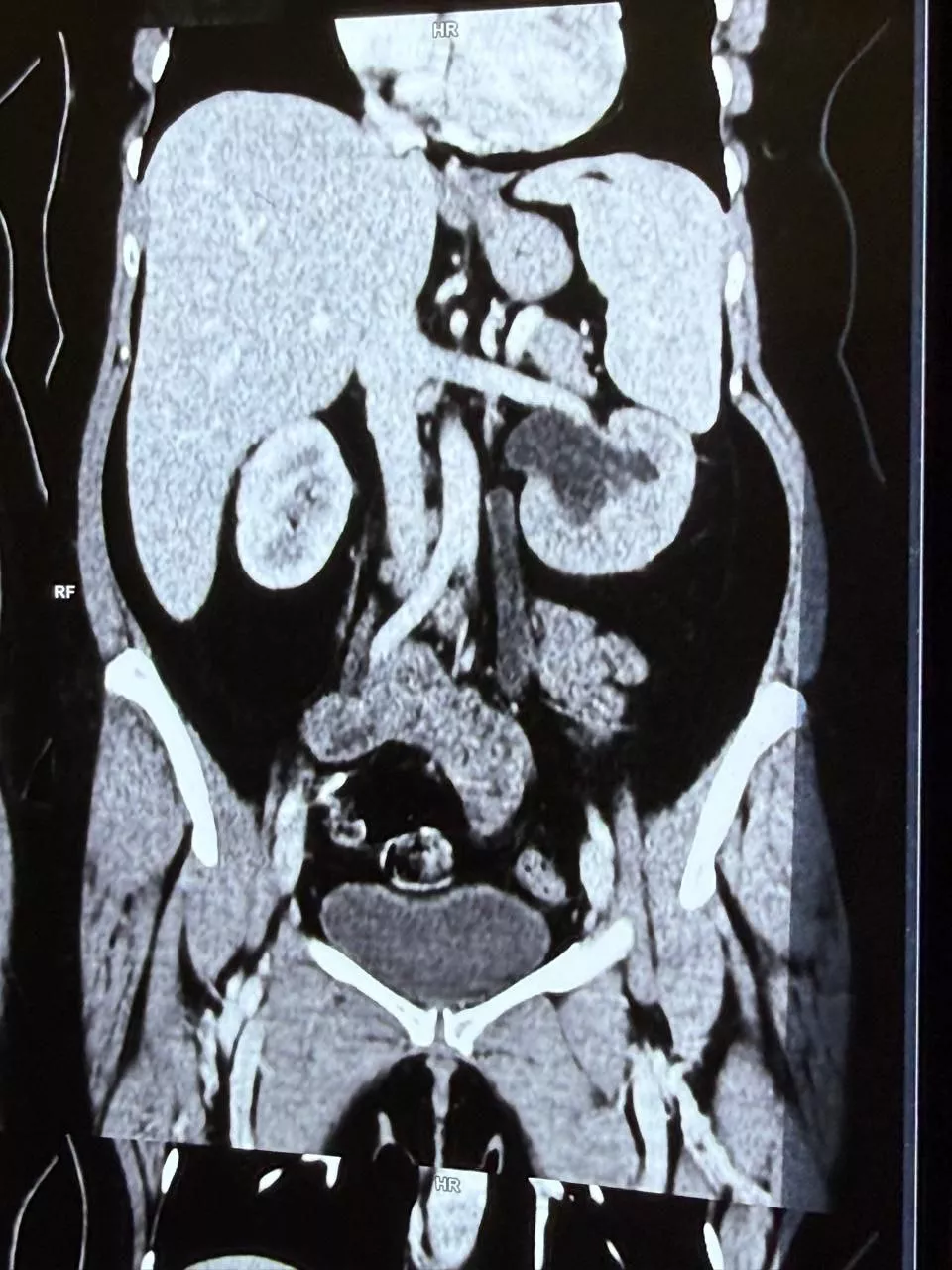
A 51-year-old woman presented to the Emergency department in the Aster RV Hospital with severe chest and abdominal pain for one week. ECG was unremarkable. 2D Echo showed a dilated aortic arch with a suspicion of a dissection flap in the aorta. CT aortogram was obtained and it showed a chronic Type B dissection of the Aorta with aneurysmal dilatation of the thoracic and the proximal descending aorta. The dissection extended from the origin of the left subclavian artery up to the origin of the Coeliac Artery (superior mesenteric artery).
There was a high risk of impending rupture due to the aneurysmal dilatation of the arch and upper descending thoracic aorta. Meticulous plan of management was done with experts from the departments of Cardiology, Cardiac Surgery, Interventional Radiology and Cardiac Anaesthesia teams. A hybrid Endovascular plus Open surgical repair of the dissecting aneurysm was then decided.
The patient then underwent the following treatment in stages by the respective teams:
1. Cardiac Surgery team performed a Left Carotid to Left Subclavian Artery Bypass grafting surgery. This was a challenging task for the CTVS surgeons as the aneurysm had extended into the root of the subclavian artery and hence it was difficult to encircle the artery completely and it could not be ligated.
2. Anaesthesia team placed a catheter in the lumbar subarachnoid space to monitor the CSF pressure. Due to the planned extent of the thoracic aorta coverage that put the patient at a high risk of paraplegia.
3. Cardiology team successfully performed Thoracic Endovascular Aortic Repair (TEVAR) with three Aortic stent grafts. The extreme angulation of the aortic arch posed a significant problem for the delivery of the stents, but was skilfully tackled by the Cardiologist.
4. A subsequent CT aortogram showed that the aneurysmal sac was still partially filling from a Type 2 endoleak from the Left Subclavian Artery. The Interventional Radiology team performed a percutaneous occlusion of the Left Subclavian Artery using a vascular plug via the Left Brachial Artery.
5. Multiple challenges were also faced by the Cardiac anaesthesia team as the patient had to go undergo three procedures within 72 hours, maintaining hemodynamic stability within a narrow range to prevent further expansion of the dissection and performing timely CSF drainage to prevent Spinal Cord ischemia. Cerebral oximetry was also used to ensure adequate perfusion of the brain.
Post operative recovery was unremarkable and she was discharged in a stable state. At 3 months, she is asymptomatic and a check CT aortogram performed that showed complete resolution of the aneurysm, obliteration of the false lumen and excellent expansion of the true lumen of the aorta. Thoracic aortic dissections and aneurysms are high risk conditions for the patient and a challenging problem for a clinician. A thorough knowledge of the clinical complexities and possible therapeutic option, precise study of the CT aortogram with accurate measurements, a combined approach with involvement of a multidisciplinary team helps the patient navigate these turbulent storms safely. This case is an example of how meticulous planning and successful collaboration between various teams- Cardiology, Cardiac surgery, Interventional radiology and Cardiac anaesthesia brought out a successful result which initially seemed farfetched.