Transverse myelitis
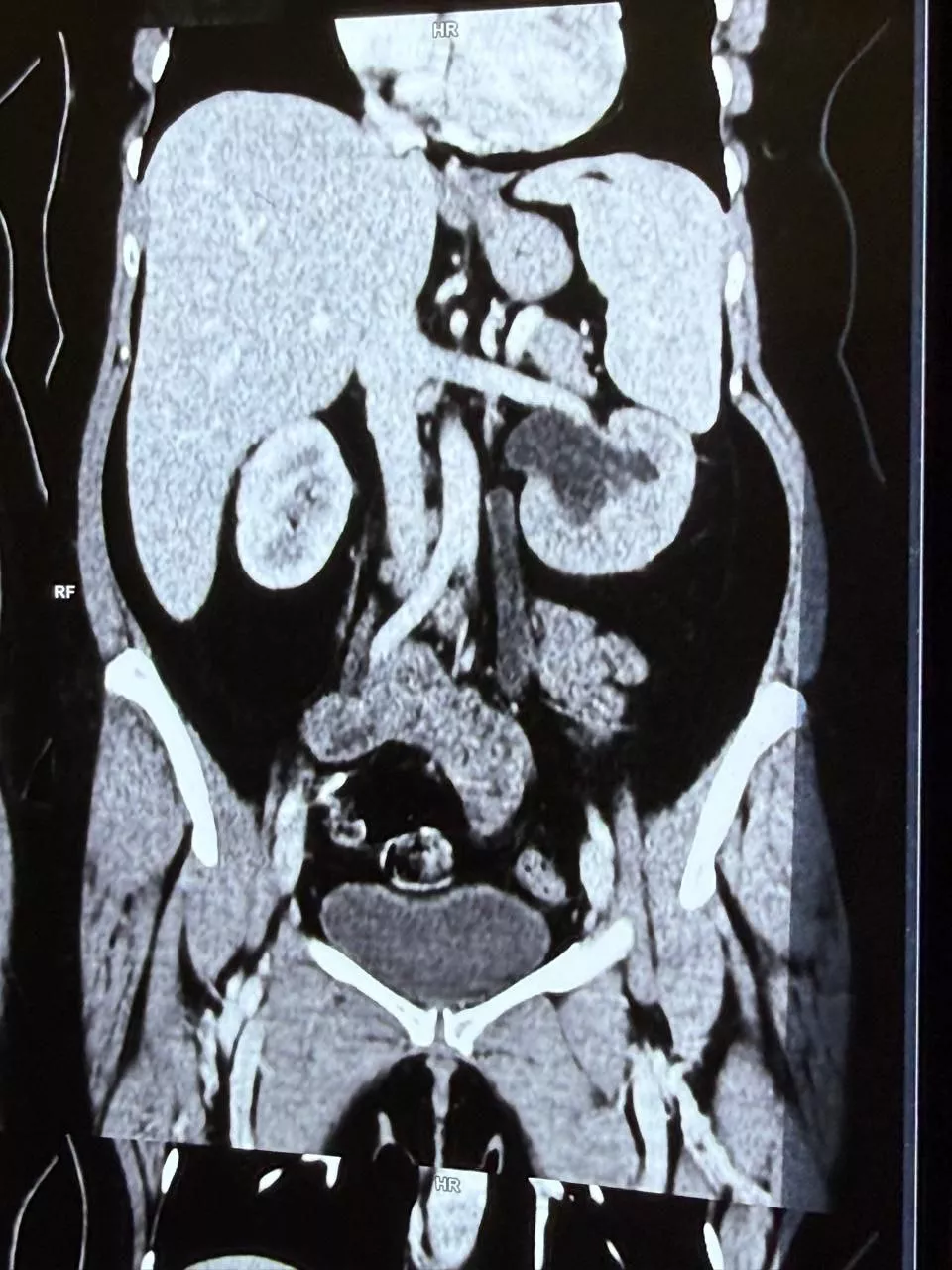
A three and half-year-old girl presented to a local hospital with an acute onset of loss of neck control and inability to hold objects in her hands, on day 3 of a febrile illness. The weakness progressed through the day with an inability to walk, followed by loss of cough reflex, poor swallowing, and pooling of secretions in the mouth. She was however conscious and able to speak. An initial CT brain scan was normal and due to persistent desaturations, she was referred to our hospital l, a tertiary-level Pediatric Hospital in JP Nagar Bangalore equipped to handle complex neurological emergencies. On arrival, she was observed to have a poor cough and gag reflex, paradoxical labored breathing with reduced air entry on the right side. Neurological examination revealed a conscious child with neck lag, absent deep tendon reflexes- upper limb, lower limb- knee jerk 2+, ankle-1+, plantar- extensor; power- 1/5 both upper limbs and 3+/5 both lower limbs. There were no obvious cranial nerve palsies apart from a weak cough and gag. The child was intubated and ventilated. Initial chest X-ray was suggestive of right hemidiaphragm palsy. An initial MRI brain and spine suggested transverse myelitis involving the central portion of the cervical cord up to the level of D2 from the cervico-medullary junction (See Fig 1-3). CSF analysis revealed HHV 6 positive with no albumin-cytologic disassociation. An extensive autoimmune panel was negative. A dose of 2g/kg IVIG and a pulse dose of methylprednisolone for 5 days was given. However, her power in both lower limbs continued to worsen. She failed a trial of extubation and following reintubation, she was unable to trigger breaths on the ventilator. A tracheostomy was done on day 6 of PICU admission and full ventilation continued. As part of her treatment, she underwent 11 cycles of plasmapheresis. She developed bowel and bladder incontinence and an overlap Guillain Barre Syndrome was considered and another dose of 2g/kg IVIG was given. The repeat CSF examination was normal. A repeat MRI 4 weeks later showed good improvement in the transverse myelitis changes (See Fig 4-5). However, the child did not show any improvement in the power of the upper and lower limbs. A nerve conduction study was done which confirmed acute motor axonal neuropathy as a co-existent condition, a rare complication of HHV 6 and similar viral infections. It was difficult to wean ventilation and the right hemi-diaphragmatic palsy persisted (See Fig 6) leading to a few episodes of ventilator-associated pneumonia which improved with antibiotics and chest physiotherapy.
The child was given Injection Rituximab for a total of 4 doses, weekly once. Steroids were gradually tapered and stopped over a total period of 8 weeks. Bowel & bladder movements improved, and power in the upper limbs gradually improved from 0 - 2. Repeated Chest X-rays showed persisting elevation of the right hemidiaphragm and serial bedside Ultrasound showed decreased excursion of the right diaphragm. Right phrenic nerve stimulation showed no response. Fluoroscopy showed a definitive persisting right diaphragm palsy. An MDT with the PICU team, pediatric surgeon, neurologist, and pulmonologist opined that diaphragmatic plication will not benefit the child and it was planned to gradually shift to BIPAP support with higher settings on the portable ventilator. The child was managed over the course of 3 months in the PICU with ongoing ventilator support and transitioned to portable BiPAP settings. Parents were trained to manage the tracheostomy and ventilator management, nutritional support via oral and NG tube feeds, and basic life support training. At discharge, the child was on BiPAP settings of pressures 16/8, rate of 35, and FiO2 of 5lpm via tracheostomy. Neurologically, she was able to speak, with some improvement in the power of her upper and lower limbs.
Transverse myelitis in association with AMAN is a rare complication reported in children following viral infections and requires a strong degree of suspicion and prompt treatment by experienced Paediatricians in JP Nagar Bangalore working within a multispecialty framework. The prognosis is expected to be a slow recovery over the years. IVIG, Steroids, Plasmapheresis, and Rituximab are the mainstay of therapeutic interventions. Vigilant intensive care to prevent hospital-acquired infections is the cornerstone for survival. The majority of patients succumb to ventilator-associated pneumonia as the mode of death. Supportive high-end care including long-term ventilation via tracheostomy, nutritional support through NG feeds, and neurorehabilitation are key to survival and gradual recovery. It requires a multispecialty PICU to manage such complex patients to provide good outcomes. Transitioning to home requires the training and commitment of families to manage the complex machine-dependent child for better survival outcomes.