Pulmonary rehabilitation is a comprehensive program that includes exercise, breathing techniques, and education to help improve lung function and quality of life in people with chronic obstructive pulmonary disease (COPD). The goal of pulmonary rehabilitation is to help people with COPD breathe more easily, stay active, and reduce the frequency and severity of exacerbations.
Pulmonary rehabilitation programs are usually conducted in a supervised setting, such as a hospital or rehabilitation center.
The program is typically tailored to the individual needs of each person with COPD and may include the following components:
-
Exercise training:
This includes aerobic exercise, such as walking or cycling, and strength training to help improve overall physical fitness and build muscle strength.
-
Breathing techniques:
These may include diaphragmatic breathing, pursed lip breathing, and other techniques to help people with COPD breathe more efficiently and reduce shortness of breath.
-
Education:
This may include information on COPD, how to manage symptoms, proper use of medications, and strategies for coping with the emotional and psychological impact of the disease.
-
Nutritional counseling:
A healthy diet can help improve lung function and overall health in people with COPD, and nutritional counseling may be provided as part of the rehabilitation program.
-
Psychosocial support:
COPD can have a significant impact on a person's emotional and psychological well-being, and pulmonary rehabilitation may include counseling or support groups to help people cope with the challenges of living with the disease.
Studies have shown that pulmonary rehabilitation can significantly improve lung function, exercise capacity, and quality of life in people with COPD. It can also reduce the frequency of hospitalizations and exacerbations, and improve overall survival. Pulmonary rehabilitation is typically recommended for people with moderate to severe COPD, but may be beneficial for anyone with the disease who is experiencing symptoms that affect their daily life.
Lung transplantation in COPD :
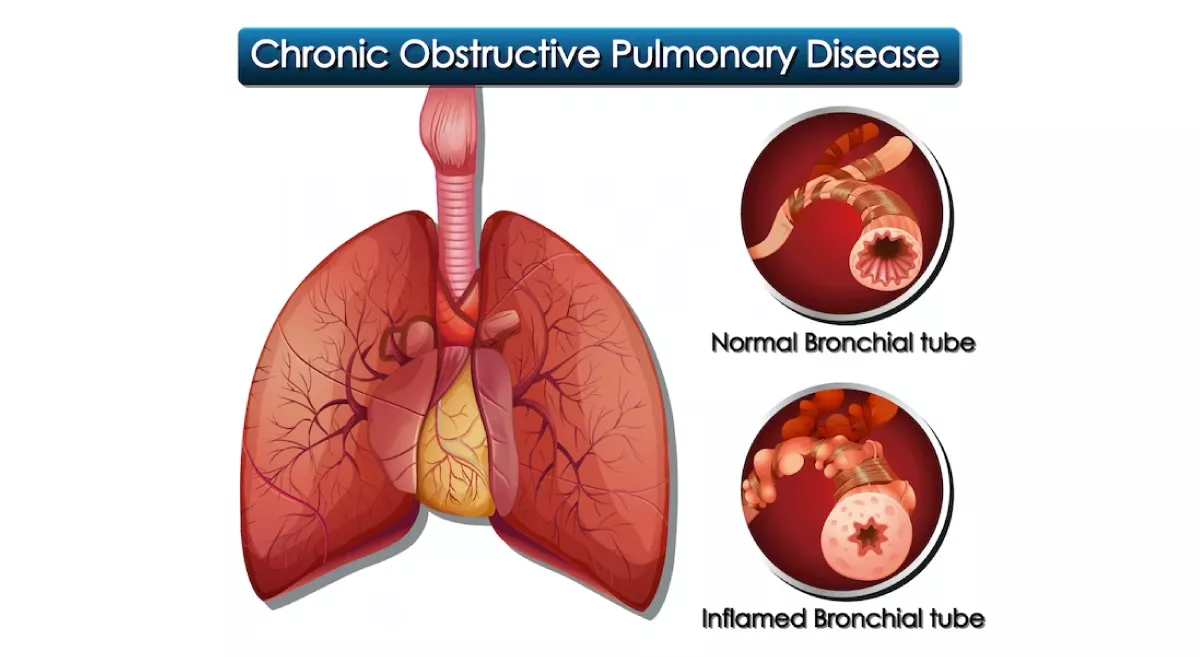
Lung transplantation is a surgical procedure that involves replacing one or both diseased lungs with healthy lungs from a donor. It is considered as a treatment option for people with end-stage COPD, which is the most severe form of the disease. End-stage COPD is characterized by very severe lung function impairment and significant symptoms despite maximal medical treatment.
Lung transplantation can provide significant benefits to people with end-stage COPD, including:
-
Improved quality of life:
Lung transplantation can relieve symptoms such as shortness of breath, fatigue, and coughing, allowing people to resume normal activities and enjoy a better quality of life.
-
Prolonged survival:
Lung transplantation has been shown to prolong survival in people with end-stage COPD.
-
Reduced hospitalization and exacerbation rates:
People who undergo lung transplantation may experience a reduced rate of hospitalization and exacerbation.
Lung transplantation is not suitable for everyone with COPD, and the decision to undergo the procedure is made on a case-by-case basis. Factors that are considered include age, overall health, severity of the disease, and the ability to adhere to the necessary post-transplant care.
After the procedure, people who undergo lung transplantation will need to take immunosuppressive medications for the rest of their lives to prevent rejection of the transplanted lungs. They will also need to undergo regular follow-up care to monitor their lung function and overall health.
Overall, lung transplantation can be a life-saving treatment option for people with end-stage COPD, but it is a major procedure with limitations, and careful consideration and evaluation is needed before deciding on this course of treatment.