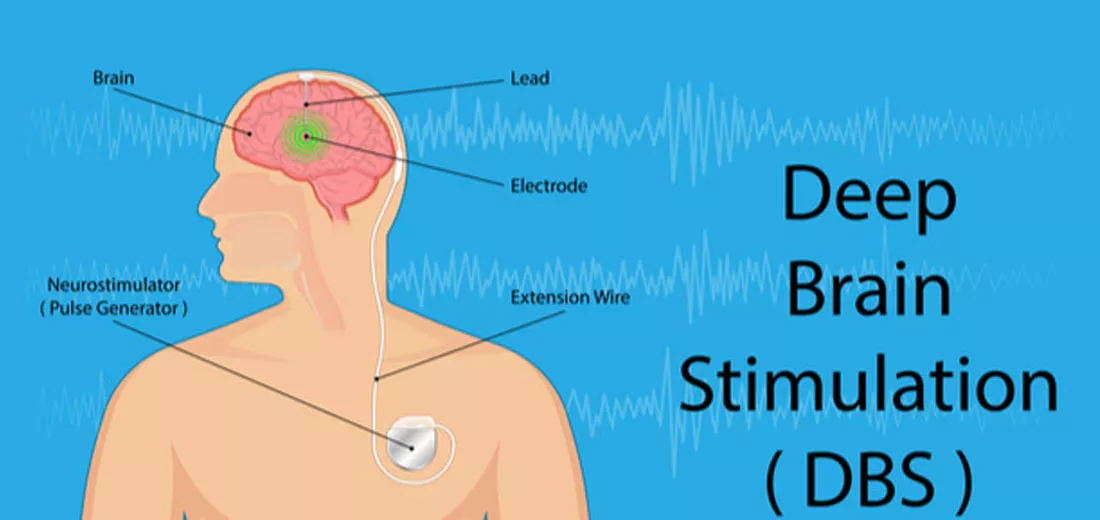
Parkinson disease is one of the most common movement disorder caused by the degeneration of dopamine producing part of the brain called the substantia nigra. As dopamine is an important neurotransmitter
Patient Stories
Our patients are our best advocates, hear the inspiring stories of their treatment journey
Blogs
The source of trustworthy health and medical information. Through this section, we provide research-based health information, and all that is happening in Aster Hospital.